Are Cold Sores Herpes? The Difference Between HSV-1 and HSV-2
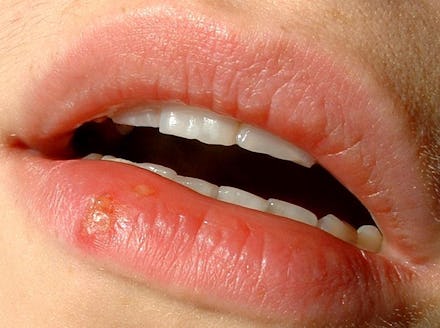
TL;DR: Yes, cold sores are herpes. And yes, they can spread to the genitals, which means they can become genital herpes.
There are two forms of the herpes simplex virus (HSV), herpes simplex-1 and herpes simplex-2. The former (HSV-1) is typically associated with oral herpes (i.e. cold sores) and is "primarily transmitted through oral-oral contact." It's also quite common: According to Herpes.com, approximately 80% of people have come in contact with HSV-1 at some point. That's not to say that 80% of people have it — exposure doesn't equal transmission — but demonstrates that this form of herpes is far from rare.
Read more:
Another important point to note: HSV-1 isn't always confined to the mouth. It can result in sores on the cheeks, nose, chin and fingers. Which helps explain both its frequency and how it can be communicated to the privates: HSV is spread through skin-to-skin contact regardless of strain, so whenever an infection site on a person's mouth, for example, comes in contact with another person's downstairs business, transmission is a possibility.
According to the Centers for Disease Control and Prevention, cases of genital herpes derived from HSV-1 are rising. However, the CDC also reported that the national percentage of people with HSV-2 (the strain that's usually responsible for genital herpes) declined between 2007 and 2010.
But — and this is a big but — there appears to be a vast difference in the ability to be transmitted between the two strains. In 2013, the Hairpin published an essay that explains the myriad difficulties surrounding a herpes diagnosis. A person with oral HSV-2 likely has genital herpes, the essay said, and runs a higher risk of passing the virus along, even when they're not showing symptoms.
HSV-1 is far more difficult to spread genital-to-genital than it is mouth-to-mouth, as Dr. H. Hunter Handsfield of the University of Washington Center for AIDS and STD told the Hairpin. Those who have HSV-1 genital herpes are not only less likely to have another outbreak, but unlikely to spread it to their partners. According to the essay, they almost never do.
Why are some doctors weary of herpes testing? There are many reasons why most doctors don't automatically test for herpes in the course of a standard STI screening. Indeed, the CDC doesn't recommend screening for people who have never shown symptoms. Why? There are many answers to that question, including (but not limited to) the potential for mental trauma, the risk of false positives and the fact that there's no cure. The waters around herpes are muddy, and while a person who's been exposed to the virus has should get tested, they should also remember that herpes isn't a death sentence, and a cold sore isn't necessarily an indication of an STI.
Correction: June 20, 2017